- World Health Organization. (n.d.). Palliative care. World Health Organization. Retrieved November 17, 2022, from https://www.who.int/teams/integrated-health-services/clinical-services-and-systems/palliative-care
- Chung, R. et al. (2017). Knowledge, attitudes, and preferences of advance decisions, end-of-life care, and place of care and death in Hong Kong. A population-based telephone survey of 1067 adults. Journal of the American Medical Directors Association; 18(4), 367.e19
- World Health Organisation. Fact Sheet No. 402: Palliative Care. 紓緩治療平台 – 主頁. (n.d.). https://www21.ha.org.hk/smartpatient/PalliativeCare/zh-hk/Home/
- General Medical Council. (2010). Treatment and care towards the end of life: good practice in decision making. Retrieved from https://www.gmc-uk.org/-/media/documents/Treatment_and_care_towards_the_end_of_life___English_1015. pdf_48902105.pdf
What is EoLC ?
紓緩治療 (Palliative Care)
According to the World Health Organization¹, palliative care is a method of caring for patients with critical illness and their families/carers, with the aim of improving their quality of life. Palliative care prevents and relieves suffering through early identification, assessment and management of pain and other physical, psychosocial or spiritual problems. Palliative care uses a cross-team approach to support patients until death. It also provides appropriate support to family members during the process and provides grief counseling after the patient’s death.
Palliative care is targeted at patients with critical illness, including cancer or other chronic diseases such as renal failure, chronic respiratory diseases, cardiovascular and neurological diseases, etc. Designed to provide holistic physical, psychological, social and spiritual care to patients and their families suffering from critical illness. The HA uses an inter-professional team, including doctors, nurses, medical social workers, clinical psychologists, physiotherapists, occupational therapists, etc., to provide appropriate palliative care services to patients and their families in an integrated service model. The purpose is to Improve their quality of life and help patients spend the last part of their lives more peacefully.
Many people in society have misunderstandings about palliative care. They believe that palliative care is equivalent to late stage care or giving up treatment², and that it is only suitable for patients who have entered a later stage of the disease or are about to die. In fact, palliative care is also applicable to the early stages of critical illness and can be used in parallel with curative treatment. It aims to relieve symptoms caused by the disease and treatment, such as pain, fatigue, asthma, nausea, depression, etc., and relieve the patient’s symptoms. of physical and mental pain. In the early stages of illness, palliative care can effectively improve patients’ quality of life and reduce unnecessary hospital admissions³. When a patient is near death, palliative care services also include late-life care. Therefore, palliative care is an indispensable part of the entire medical care process.
安寧照顧 (End-of-Life Care)
When a patient is diagnosed with an incurable disease and is likely to die within the next 6 to 12 months. Palliative care generally refers to providing palliative care to such patients until the end of life (palliative care includes but is not limited to palliative care), including:
- Imminent death (expected to die within hours or days) and the following persons
- Have a severe and progressive life-limiting disease (e.g. advanced cancer, advanced motor neuron disease
- 整體身體虛弱和同時患有多種疾病,預計病人會在 6 至 12 個月內死亡
- 患有可能因急性病發而導致死亡的疾病
安寧照顧旨在幫助病人舒適地走完人生最後一程,達致安然善別。同時,安寧照顧會為病人減輕疼痛、控制症狀以及提供心理社交和心靈支援,提升病人及家人的生活質素 ; 還包括各項醫療和社會照顧服務,例如疾病的專科治療、紓緩治療和寧養照顧等。
寧養照顧 (Hospice Care)
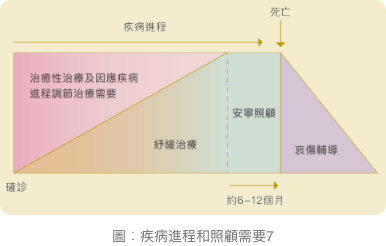
寧養照顧相等於臨終關懷,主要針對的對象為臨終病人(即預期壽命一般少 於 6 個月或更短),以及已經採取過一切治癒性治療的病人5 。寧養照顧的首要目標會由延長壽命過渡至提升病人臨終前的生活質素。寧養照顧的服務包括 紓緩照顧以及其他全面的照顧和治療,例如藥物治療、心理社交和心靈上的支援等。此外,寧養照顧亦會照顧家人在面對疾病和死亡過程中的各項需要,協助他們調適生活上的困難
- Hospital Authority. (2017). HA strategic service framework for palliative care. Retrieved from https://www.ha.org.hk/haho/ho/ap/PCSSF_1.pdf
- Institute of Medicine of the National Academies. (2015). Dying in America: Improving quality and honouring individual preferences near the end of life. Washington, DC: The National Academies Press.
- 香港中文大學賽馬會老年學研究所 (2020) 。<<安寧服務培訓及教育計劃:醫護人員培訓手冊>>。香港︰作者。
「預設照顧計劃」 (Advance Care Planning, ACP)
一般「預設照顧計劃」的溝通對象是精神上能夠自決的成年病人,並歡迎家屬參與。病人可表達本身對未來醫療或個人照顧的意願,或作出拒絕接受維生治療的「預設醫療指示」。
在醫院管理局,「預設照顧計劃」也涵 蓋精神上不能自決的病人及未成年病人。 醫護人員與病人家屬可根據病人的最佳利益,謀求共識,為病人計劃未來的醫 療或個人照顧。
「預設照顧計劃」的目的
- 精神上有行爲能力及妥為知情的病人可:
- 表達其價值觀、信念和願望;
- 表達本身對未來醫療或個人照顧的意向;
- 作出拒絕接受維持生命治療(包括「不作心肺復甦術」)的預設醫療指示#;
- 委托一名家庭成員作為主要聯絡人,以便日後作諮詢。
- 精神上無行爲能力的成年病人或未成年病人,其家人與醫護團隊可根據病人的最 佳利益,同時顧及病人曾表達的願望、意向和價值觀,並衡量現有選擇的好處、 風險和負擔,尋求共識,為病人制訂未來的醫療或個人照顧計劃。
- 當病人日後病情惡化,病人及其家人可以有較充足心理準備。
「預設照顧計劃」的好處
實踐病人知情權 :
體現病人自主 :
符合病人最佳利益 :
避免日後爭議 :
促進家庭關係 :
減少臨終痛苦:
預設醫療指示 (Advance Directive, AD)
「維持生命治療」指任何有可能延遲病人死亡的治療,例子包括使用心肺復甦法、人工輔助呼吸、血液製品、心臟起搏器及血管增壓素、為特定疾病而設的專門治療(例如化學治療或透析治療)、在感染可能致命的疾病時給予抗生素、以及人工營養及流體餵養。(人工營養及流體餵養指透過導管餵飼食物和水份。)香港現時並沒有法例規定預設醫療指示要以何種形式表達,但是醫院管理局有特定的「預設醫療指示」表格,供醫管局病人使用,表格涵蓋以下情況:
第1類情況「病情到了末期」
第2類情況「持續植物人狀況或不可逆轉的昏迷狀況」
第3類情況「其他晚期不可逆轉的生存受限疾病」
見證人




